Joplin (KS & MO) Preferred Managed Choice (Open Access).Joplin (KS & MO) Preferred Aetna Choice POS II.Aetna Open Access® Managed Choice® POS (Aetna HealthFund®).Aetna Open Access® Elect Choice® EPO (Aetna HealthFund®).Aetna Health Network Only℠ (Open Access).Aetna DE Bronze, Silver and Gold HNOption.Aetna DE Bronze, Silver and Gold HNOnly.Aetna DC Bronze, Silver and Gold HNOnly.Aetna Choice® POS II (Aetna HealthFund®).We Are In-Network with the following Aetna plans: * Most Aetna HMO Plans require that their members have a referral from their Primary Care Physician prior to having services covered at an Urgent Care. Reviewing your medical expenses may help you determine the coverage that is best for you and your family.Physicians Immediate Care is in-network with Aetna Health Insurance. Review your claims and expenses for the previous year at (login required). You want to be able to visit specialists without getting referrals from a PCP.You are open to controlling your health care costs by using in-network providers and receiving higher benefits.You need open access to any licensed health care provider.This includes higher per paycheck premiums. You are willing to pay higher out-of-pocket costs in exchange for more choice.You should choose the Choice POS II plan if: Click here to learn more about prescription benefits. This program includes a Formulary Management Program that uses a “four-tier” copayment approach to covered drugs and is designed to control cost for you and the plan. When you enroll in one of the Aetna medical plan options, you’ll automatically have prescription drug coverage through Aetna and Express Scripts. To find preferred providers near you, visit Prescription Drug Benefits Facilities such as hospitals, urgent care centers, and labs also belong to the network. It consists of primary care physicians and specialists ranging from cardiologists, podiatrists, and OB/GYNs to oncologists, ophthalmologists, and orthopedists. The Aetna Choice network is large and comprehensive. You’ll be billed for any amount that exceeds the reasonable charge. If he or she doesn’t, benefits will be paid at the lower, out-of-network level AND only up to what Aetna determines to be the reasonable charge for the service. If your doctor refers you to another provider (such as a specialist), be sure to ASK if the provider belongs to the network.
AETNA CHOICE POS II FREE
While you are free to use any provider, you save money when you use in-network providers. In addition, you must file your own claims and call Aetna when your doctor recommends care that must be precertified. The plan pays a smaller share of your expenses. Out-of-Network Benefits - If you use an out-of-network provider, you will receive a lower level of benefits and you must meet a higher deductible.In addition, the in-network provider files claims for you and takes care of the plan’s precertification requirement(s) for hospital admissions. For other services, you pay a lower deductible and the plan pays a larger share of your expenses. In-Network Benefits - When you use in-network providers, you pay a fixed dollar amount, called a copayment (or copay), for doctor’s office visits and routine exams.The Aetna Choice POS II Plan has two levels of benefits:
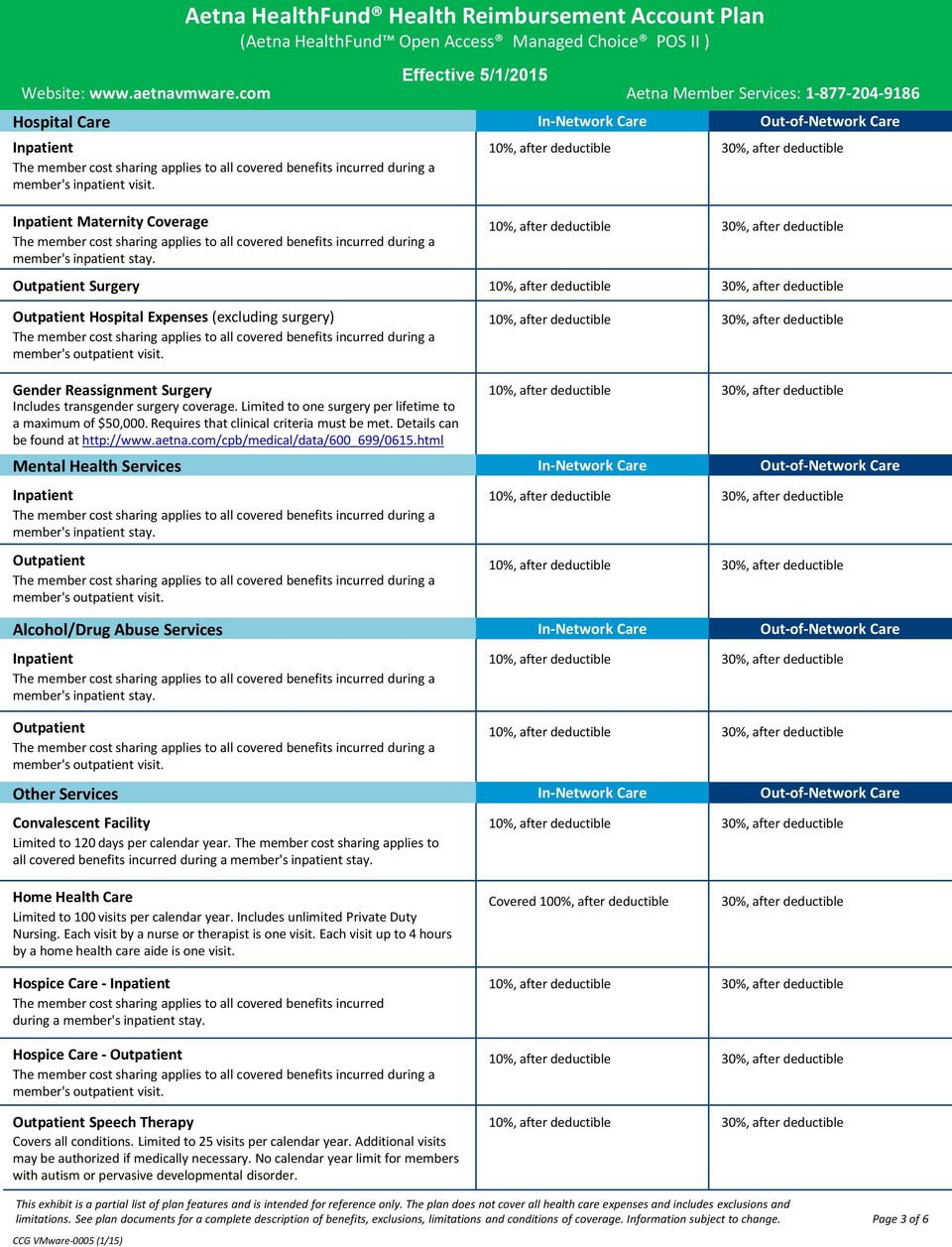
When you need care, simply choose the appropriate doctor and make an appointment. You are not required to select a primary care physician (PCP) and no referrals are required for specialty care. Under the Aetna Choice POS II Plan, you may receive care from any licensed health care provider. This plan offers both in-network and out-of-network benefits however, the plan’s reimbursement is higher when you use an in-network provider.

It provides the highest level of benefits. The Aetna Choice POS II Plan is a network plan that gives you the freedom to select any licensed provider when you need care.
